
Paths to Practice Perfection
Tips for Managing VLUs: Decrease Inflammation/Infection, Control Exudate, and Control Edema
Tips for Managing VLUs: Decrease Inflammation/Infection, Control Exudate, and Control Edema

Introduction
Venous Leg Ulcers (VLUs) are the most common ulcer of the lower limb, affecting approximately 1% of the population and 3-8% of people 80 years or older.1 VLUs are typically located on the gaiter region of the lower leg. These wounds are typically shallow and irregular in shape. VLUs are often heavily exudative as chronic venous hypertension can cause the vein walls to eventually leak fluid and proteins out resulting in increased exudate.2
Strategies to manage highly exudative VLUs include, periwound skin protection, primary and secondary dressing selection, and the use of correct compression.
Clinicians should follow an evidence-based treatment approach for VLUs which includes wound hygiene, exudate management, compression therapy, and appropriate infection/inflammation control. The patient may also require a vascular consult to manage the underlying venous insufficiency.
Periwound Protection
VLUs are usually highly exudative, as such, managing exudate while protecting the periwound skin is an important component of the treatment plan. Dressings that can handle high levels of exudate and wick exudate off the periwound skin all while maintaining an optimal wound healing environment are ideal. Superabsorbent dressings such as the 3M™ Kerramax Care™ Super-Absorbent Dressings wick fluid both horizontally and vertically, allowing the moisture to be retained in the dressing and not sitting on the periwound skin. Kerramax Care Dressings can be placed under multi-layer compression for added absorbency of these highly exudative VLUs.

3M™ Kerramax Care™ Super-Absorbent Dressings combine a super-absorbent core with 3M™ Exu-Safe™ Technology that absorbs and retains high levels of exudate, while supporting patient comfort.
Primary and Secondary Dressings
The ideal primary dressing is one that conforms to the wound surface, prevents dead space, and absorbs a large amount of exudate. The goal is to wick the exudate away from the wound surface, preventing maceration.
Using a collagen matrix with oxidized regenerated cellulose (ORC) and silver-ORC (3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver) may be utilized to help prepare the wound and help optimize the moist wound environment, and promote granulation.3 The silver-ORC dressing in the wound serves as an antibacterial barrier and has been shown to reduce bacterial bioburden and growth along with helping support a moist wound environment conducive to healing.4 The ORC component has shown to reduce protease and matrix metalloproteinase levels in chronic wound fluid which can be elevated in chronic wounds such as VLUs.3,5
3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver

The silver-ORC in Promogran Prisma Matrix helps to provide a barrier to bacteria in the dressing. 3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver helps deal with the inflammation and the inflammatory environment.6*
Compression Therapy
Compression therapy of 40 mmHg at the ankle is the gold standard for the treatment of VLUs. Compression therapy helps to reduce lower leg edema, improve venous return, and aide in wound healing.7 There are many options for compression therapy, single layer, multi-layer, long stretch, short stretch, and stockings. The type of compression therapy used should be based on the patient’s needs. One multi-layer compression system that can provide compression 35-40 mmHg for patients with an ankle brachial pressure index ABPI > 0.8 is the 3M™ Coban™ 2 Two-Layer Compression System. For patients with ABPI >0.5 the 3M™ Coban™ 2 Lite Two-Layer Compression System may provide clinical benefits.8 This multi-layer compression system can provide sustained therapeutic compression for 4-7 days depending on condition.

3M™ Coban™ 2 Two-Layer Compression System provides effective compression therapy, which has been shown to contribute to effective VLU management through edema reduction, decreased pain, and improvement in a patient’s daily activities.8,9
Case Presentation
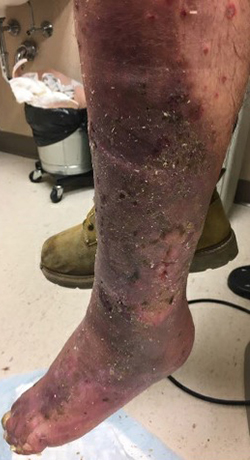
A 56-year-old male presented with a left leg wound (Figure 1) that had been present off and on for 10 years. The patient stated that the ulceration started from a brown recluse spider bite. His medical history included paraplegia for 33 years post motor vehicle accident. The patient has worn compression stockings in the past. Examination of the left lower leg revealed a large wound with copious amounts of drainage. Hemosiderin staining was noted, pulses were all palpable. A venous insufficiency ultrasound was completed and showed reflux and insufficiency in the greater saphenous vein (GSV). After wound evaluation and ultrasound, the wound was diagnosed as a VLU.
The patient underwent weekly visits to the wound center where he received wound cleansing and debridement. Application of Promogran Prisma Matrix followed by a Kerramax Care Dressing. The patient was then wrapped from toes to knee with the Coban 2 Compression System. The wound improved and the patient underwent venous ablation of the GSV.
Throughout treatment, reduced amounts of exudate were noted along with the development of robust granulation tissue, and a notable decrease in wound size (Figures 2-6). At day 45, the patient’s wound was completely healed, and he was transitioned to his home with compression stockings.

Figure 1. Wound at presentation

Figure 2. Wound after 7 days of 3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver, 3M™ Kerramax Care™ Super-Absorbent Dressing, and 3M™ Coban™ 2 Two-Layer Compression System.

Figure 3. Wound after 14 days of 3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver, 3M™ Kerramax Care™ Super-Absorbent Dressing, and 3M™ Coban™ 2 Two-Layer Compression System.

Figure 4. Wound after 21 days of 3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver, 3M™ Kerramax Care™ Super-Absorbent Dressing, and 3M™ Coban™ 2 Two-Layer Compression System.

Figure 5. Wound after 28 days of 3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver, 3M™ Kerramax Care™ Super-Absorbent Dressing, and 3M™ Coban™ 2 Two-Layer Compression System.

Figure 6. Wound after 35 days of 3M™ Promogran Prisma™ Collagen Matrix with ORC and Silver, 3M™ Kerramax Care™ Super-Absorbent Dressing, and 3M™ Coban™ 2 Two-Layer Compression System.
Conclusion
This case demonstrated an evidence-based approach for the treatment of a venous leg ulceration. Patients with VLUs can be challenging to treat due to heavy exudate, pain, and underlying inflammation/infection. Wound debridement, advanced wound care dressings, and compression therapy can be used to manage these wounds. Once closed it is important to educate our patients that lifelong treatment with compression garments is needed to prevent recurrence.
Do you have questions regarding this case study?
Connect with a 3M Account Representative to discuss how 3M can help you offer the continuum of care to your patients.
Patient data and photos courtesy of Emily Greenstein, APRN, CNP, CWON, FACCWS.
Note: Emily Greenstein was a paid consultant for 3M products at the time of this case study.
As with any case study, the results and outcomes should not be interpreted as a guarantee or warranty of similar results. Individual results may vary depending on the patient’s circumstances and condition.
NOTE: Specific indications, contraindications, warnings, precautions, and safety information exist for these products and therapies. Please consult a clinician and production instructions for use prior to application. Rx only.
Footnote:
*in-vitro
© 2022 3M. All rights reserved. 3M and the other marks shown are marks and/or registered marks. Unauthorized use prohibited.
References:
- Posnett J, Gottrup F, Lundgren H, Saal G. The resource impact of wounds on health-care providers in Europe. J Wound Care. 2009;18(4):154-161.
- Simon DA, Dix FP, McCollum CN. Management of venous leg ulcers. BMJ. 2004;328(7452):1358-1362.
- Gottrup F, Cullen B, Karlsmark T, Bischoff-Mikkelsen M, Nisbet L, Gibson M. Randomized controlled trial on collagen/oxidized regenerated cellulose /silver treatment. Wound Repair & Regeneration 2013;21: 1-10.
- Wu S, Applewhite AJ, Niezgoda J, et al. Oxidized regenerated cellulose/collagen dressings: review of evidence and recommendations. Adv Skin Wound Care. 2017;30(11S):S1-S18.
- Cullen B, Watt PW, Lundqvist C, et al. The role of oxidized regenerated cellulose/collagen in chronic wound repair and its potential mechanism of action. Int J Biochem Cell Biol. 2002;34(12):1544-1556.
- Gibson M, et al. Can natural materials be optimized to improve wound environment? Presented at European Wound Management Association; May 12-14, 2015; London, UK.
- O’Meara S, Cullum NA, Nelson EA. Compression for venous leg ulcers. Cochrane Database Syst Rev. 2009(1):CD000265.
- Moffatt C, Edwards L, Collier M, et al. A randomized controlled 8-week crossover clinical evaluation of the 3M™ Coban™ 2 Layer Compression System versus Profore™ to evaluate product performance in patients with venous leg ulcers. Int Wound J. 2008;5(2); 267–279.
- Mosti G, Crespi A, Mattaliano V. Comparison Between a New, Two-component Compression System with Zinc Paste Bandages for Leg Ulcers Healing: A Prospective, Multicenter, Randomized, Controlled Trial Monitoring Sub-bandage Pressures. Wounds. 2011;23(5):126–134.


Comments
There are 0 comments for this article